Module 1 : Anatomy and Physiology
Introduction
This module provides an overview of the anatomy and physiology of the gastrointestinal system. It is important that you understand the physical structures and normal functions of the GI system, as we will be discussing GI pathophysiology and pharmacology later in the course.
Module Structure
This module is divided into two sections:
SECTION 1: Overview of the Gastrointestinal System
SECTION 2: Anatomy and Physiology
SECTION 1: Overview of the Gastrointestinal System
Learning Objectives
After reading this section, you should be able to:
-
- State the principal functions of the gastrointestinal system.
- List the anatomical parts of the gastrointestinal tract and the glandular organs associated with the gastrointestinal system.
- Describe the four basic processes performed by the gastrointestinal system.
Principal Function of the GI System
The principal function of the GI system is to break down large complex components of food (fats, proteins, carbohydrates) to simpler forms that can be absorbed. These molecules are distributed, via the circulatory system, to body cells to be used for energy, tissue production and repair, and for the maintenance of body functions.
The GI system also excretes any undigested material and some of the body’s waste products.
Components of the GI System
The GI system consists of two distinct components:
-
-
- the GI tract
- the GI glandular organs
-
1) Anatomical parts of the GI tract
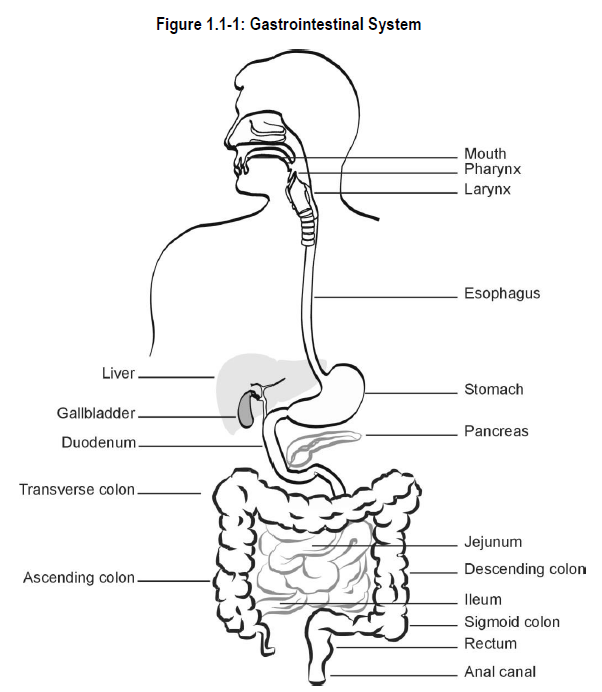
The GI tract is essentially a continuous hollow tube that is approximately 10 metres (30 feet) long. It consists of the following basic anatomical parts:
-
-
- mouth
- pharynx (throat)1
- esophagus (food pipe)2
- stomach
- small intestine (duodenum, jejunum, ileum)
- large intestine (cecum, ascending colon, transverse colon, descending colon, sigmoid colon)
- rectum
- anal canal
-
2) GI glandular organs
The GI glandular organs secrete or release substances via ducts into the GI tract and aid in the breakdown of food3. The GI glandular organs include:
-
-
- salivary glands
- liver
- gallbladder
- pancreas
-
See Figure 1.1-1.
General Physiology of the GI System
There are four basic processes performed by the GI system to accomplish its functions.
1) Digestion
Digestion is the mechanical and chemical breakdown of food into smaller molecules that can be used by the body.
2) Secretion
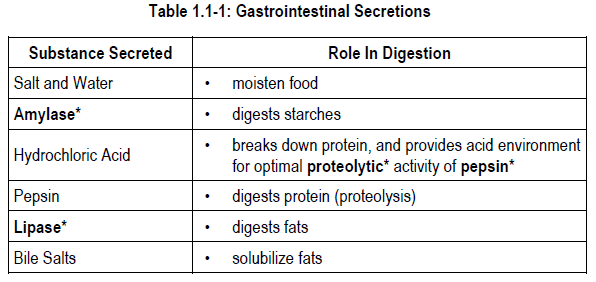
Secretion of various substances by different parts of the GI system aids the process of digestion. Some examples of GI secretions and their role in digestion are listed in Table 1.1-1.
3) Absorption
Absorption is the movement of molecules produced by digestion from the GI tract into the blood (or lymph*). The primary site of absorption is the small intestine. Molecules such as monosaccharides (i.e., simple sugars such as glucose and fructose), fatty acids, amino acids, vitamins, minerals and water cross the epithelial cells* of the small intestine and enter the blood.
4) Motility
The GI system moves food, undigested residue and wastes through rhythmic waves of muscular contraction and relaxation known as peristalsis*. Muscle contraction in the GI tract is controlled by the autonomic nervous system*.
SUMMARY — SECTION 1: Overview of the Gastrointestinal System
The two main functions of the gastrointestinal (GI) system are:
-
-
- break down food to forms that can be absorbed by body cells
- excretion of undigested material and some waste products
-
The GI tract consists of the following anatomical parts:
-
-
- mouth
- pharynx
- esophagus
- stomach
- small intestine (duodenum, jejunum, ileum)
- large intestine (cecum, ascending colon, transverse colon, descending colon, sigmoid colon)
- rectum
- anal canal
-
The GI glandular organs secrete or release substances via ducts into the GI tract. The GI glandular organs include:
-
-
- salivary glands
- liver
- gallbladder
- pancreas
-
Four basic processes are performed by the GI system to accomplish its functions:
-
-
- digestion
- secretion
- absorption
- motility
-
PROGRESS CHECK — SECTION 1: Overview of the Gastrointestinal System
1.
What are the main functions of the GI system?
______________________________
______________________________
2.
The two distinct components of the GI system are the _____________ and the ______________.
3.
Indicate whether each of the following is true or false.

4.
Match the GI system secretions in Column A with the corresponding role in digestion in Column B.

PROGRESS CHECK ANSWERS— SECTION 1: Overview of the Gastrointestinal System
1.
The GI system breaks down large complex components of food to simpler forms which can be absorbed and distributed to body cells via the circulatory system, and aids in the excretion of undigested material and some waste products.
2.
The two distinct components of the GI system are the GI tract and the GI glandular organs.
3.
1) False
The four basic processes of the GI system are digestion, secretion, absorption and motility.
2) True
3) False
The GI glandular organs include the gallbladder, the liver, the salivary glands and the pancreas, but not the adrenal glands. The adrenal glands are part of the endocrine system.
4) True
5) False
The GI tract consists of 8 basic anatomical parts: the mouth, pharynx, esophagus, stomach, small intestine, large intestine (colon), rectum and anal canal.
6) True
4.

SECTION 2: Anatomy and Physiology
Introduction
Throughout this section we will review the anatomy and physiology of the various components of the GI system.
Additional detail is provided regarding hydrochloric (HCl) acid secretion and motility, as these GI functions are most often subject to pharmacological intervention.
Learning Objectives
After reading this section you should be able to:
-
-
- Describe the function of the anatomical parts of the gastrointestinal (GI) tract.
- Describe the function of the secretions produced by the glandular organs of the GI tract.
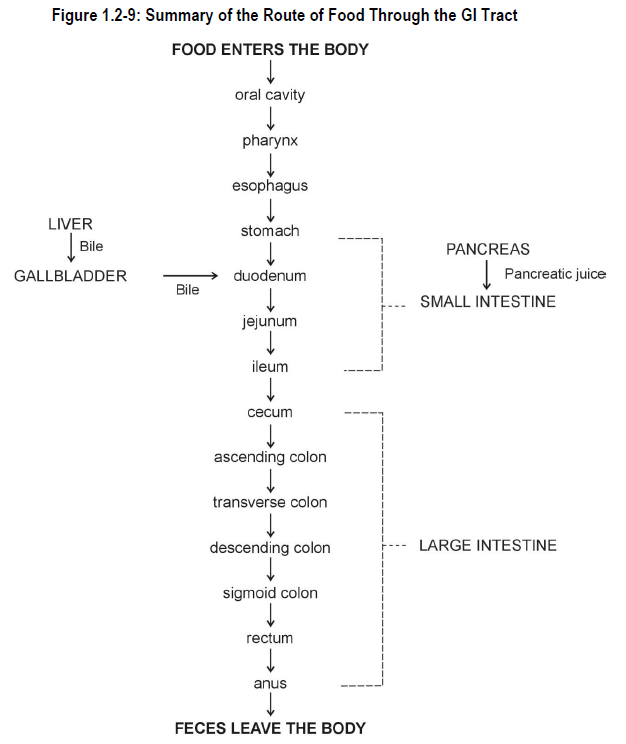
- Describe the movement of food through the GI tract.
- Describe the absorption of nutrients from the GI tract.
-
SECTION 2A: Anatomical Parts
Upper GI Tract
1) Mouth
The process of digestion, both mechanical and chemical, begins in the mouth with mastication*. Mastication breaks food down into smaller pieces and mixes them with saliva to form a bolus* that can be swallowed.
2) Pharynx
The pharynx is a muscular tube that serves as a passageway for food from the mouth to the esophagus. The pharynx is also the passageway for air from the nose to the larynx (voice box) and respiratory airways.
3) Esophagus
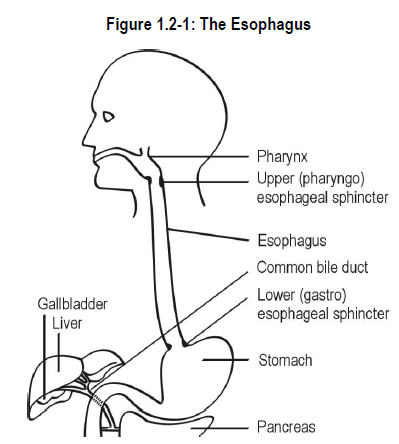
The esophagus is a hollow muscular tube approximately 25 centimetres (10 inches) long. The esophagus passes through the chest cavity and into the abdomen, connecting the pharynx and the stomach. See Figure 1.2-1.
The primary function of the esophagus is to propel food or fluid from the pharynx into the stomach by peristalsis. The esophagus possesses no significant secretory or absorptive functions.
At both the junction of the pharynx and esophagus, and the stomach and the esophagus, there are sphincters* that keep the esophagus closed except during the act of swallowing. The primary function of these esophageal sphincters is to provide a pressure barrier at each end of the esophagus.
The upper esophageal sphincter (or pharyngoesophageal sphincter) prevents:
-
-
- air from entering the esophagus during inspiration
- retrograde flow of esophageal contents back into the pharynx
-
The lower esophageal sphincter (gastroesophageal sphincter) prevents reflux* of stomach contents back up into the esophagus.
GI Tract Wall
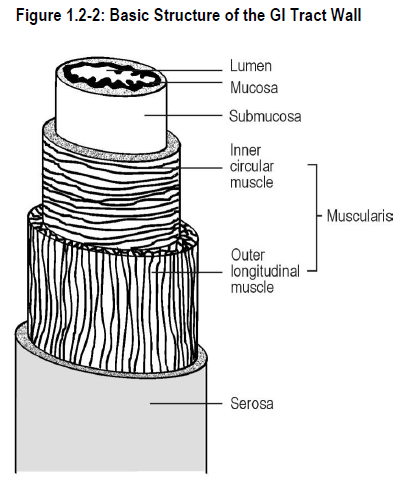
Starting at the esophagus, the walls of the GI tract have a similar basic structure, which is modified along the tract for special functions. See Figure 1.2-2.
The GI tract wall consists of four layers from deep (nearest the gut lumen) to superficial are:
1) Mucosa
The mucosa is the inner, moist membrane that lines the lumen*. The mucosa consists primarily of epithelial cells, which provide a protective barrier to the other layers of the GI tract wall. In some sections of the GI tract, such as the stomach and small intestine, the mucosa contains different secretory cells which secrete digestive enzymes*, mucus and protective substances, such as prostaglandins*.
2) Submucosa
The submucosa is the soft connective tissue layer just beneath the mucosa containing blood vessels, nerve endings and lymphatic vessels. The esophageal submucosa contains mucus-secreting glands. In the small intestine, dissolved nutrients are absorbed into the blood and lymph vessels of the submucosa.
3) Muscularis
The muscularis is the muscle layer made up of a longitudinal smooth muscle* outer layer and an inner circular layer consisting of both smooth and striated muscle*. The muscle fibres of the muscularis are arranged in layers:
1) an inner layer of fibres arranged circularly
2) an outer layer of fibres arranged longitudinally
3) an oblique (diagonal) layer (found in the stomach only)
The contraction of these muscles produces the motions of peristalsis and segmentation.
4) Serosa
The serosa (or visceral peritoneum) is the outermost layer of the GI wall, which consists of a single layer of watery, fluid producing cells. It is absent from the esophagus.
Other than the mucosa, all the layers of the GI tract wall contain networks of nerve fibres that are part of the autonomic nervous system.
Stomach
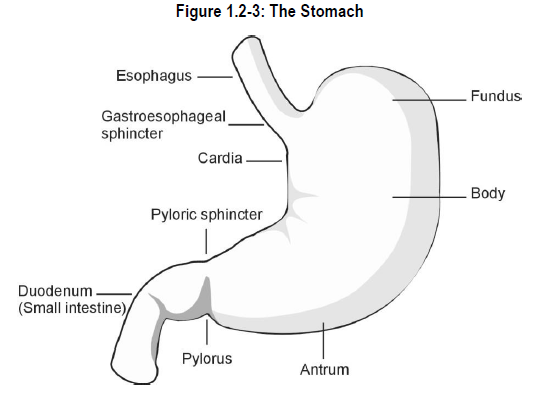
The stomach is a pouch-like structure approximately 25 centimetres (10 inches) long located between the esophagus and duodenum. For descriptive purposes, the different parts of the stomach have been named as follows:
-
-
- cardia (also called the cardiac region) – upper right-hand portion around the gastroesophageal sphincter
- fundus – expanded part of the stomach lateral to the cardia
- body – midportion of the stomach
- antrum* and pylorus* – terminal part of the stomach which connects to the small intestine
-
See Figure 1.2-3.
The stomach performs three main functions:
-
-
- stores food after a meal – After eating a meal, it may take as long as 2-6 hours for the stomach to empty.
- mixes food with gastric* secretions (acids and enzymes) that dissolve and partly digest food to produce a semisolid mixture called chyme*
- regulates delivery of the partially digested food (chyme) to the small intestine
-
The mucosa and the muscularis of the stomach are specially adapted to perform the organ’s functions.
The protection of the gastric mucosa against gastric secretions, and against noxious agents present in ingested material, is accomplished in two ways:
-
-
- a protective mechanism
- a repair mechanism
-
The protective mechanism consists of a thick, viscous, alkaline* mucus layer measuring over 1 millimetre thick, referred to as the gastric mucosal barrier. The mucous cells continuously secrete mucus and are the most numerous cell type found in the gastric mucosa.
The repair mechanism of gastric mucosal protection refers to the rapid turnover of gastric mucosal cells. The entire stomach mucosa is replaced in 1 to 3 days allowing for rapid regeneration of damaged surface epithelium*.
Pancreas
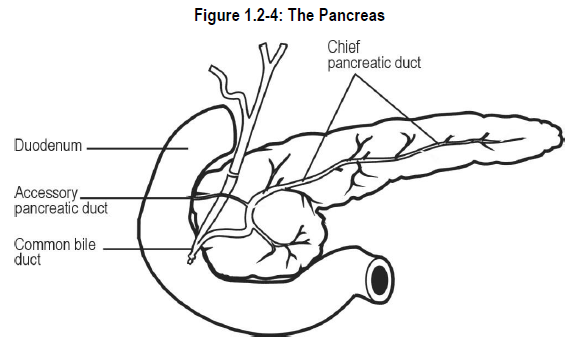
The pancreas is a large, elongated organ that lies transversely across the upper abdomen and behind the stomach. See Figure 1.2-4.
The pancreas has both endocrine* and exocrine* functions. The exocrine functions of the pancreas are relevant to the study of the GI system and include:
-
-
- the secretion of digestive enzymes (Trypsin,Lipase, Amylase) that digest fats, proteins and carbohydrates into simpler substances
- the secretion of bicarbonate ions to neutralize the highly acidic chyme from the stomach to:
– provide a favourable pH* that allows digestive enzymes to work
– protect the walls of the small intestine
-
The pancreas has an extensive ductal system that drains its exocrine secretions into the duodenum.
To visualize the pancreas, imagine a bunch of grapes. Each grape represents a gland. Each gland (grape) is attached by a duct (branch) to the chief pancreatic duct (the main branch).
The pancreatic duct crosses the entire length of the pancreas and drains the pancreatic exocrine secretions into the common bile duct and finally into the duodenum.
Liver
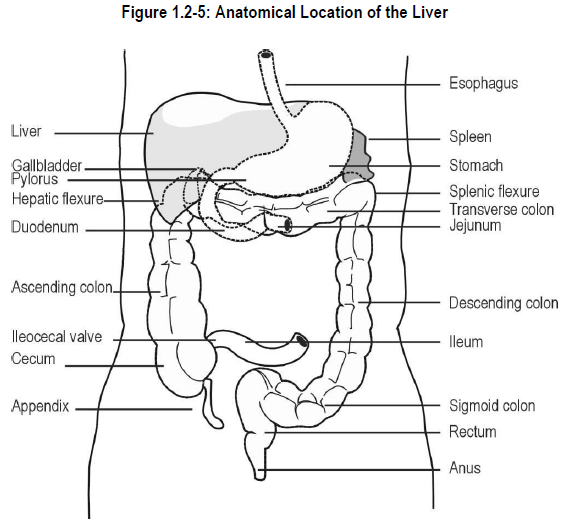
The liver, the largest gland in the body, is a wedge-shaped organ occupying the uppermost part of the abdominal cavity. See Figure 1.2-5. Most of the liver is protected by the lower right rib cage.
The liver is a very vascularized organ and has a unique blood supply called the hepatic portal system. The liver receives blood from both the portal vein and the hepatic artery.
The portal vein receives the blood flow from the intestinal tract. This supply system means that the liver has the first chance to process nutrients and drugs from the blood stream after the blood leaves the intestine.
The liver performs many metabolic and regulatory functions including:
-
-
- nitrogen and protein metabolism*
- bile acid formation and secretion (to aid fat digestion)
- bilirubin* metabolism and storage of iron and Vitamins A, B12, and D
- carbohydrate storage/blood sugar control
- hormone metabolism
- drug and toxin metabolism (detoxification)
- synthesis of serum proteins including:
– albumin*
– lipoproteins*
– clotting factors
– transport proteins
-
The primary digestive function of the liver is the production and secretion of bile*.
Gallbladder
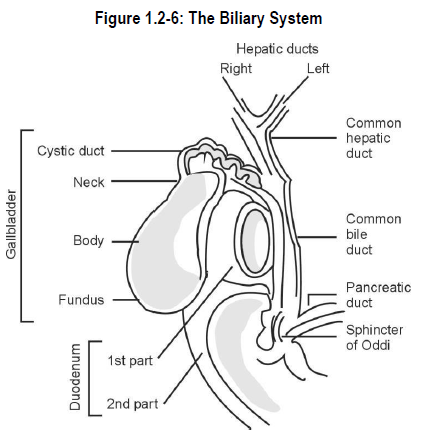
The gallbladder is a pear-shaped organ that lies in a depression on the lower side of the right lobe of the liver. See Figure 1.2-6.
The gallbladder contracts intermittently during meals to release bile into the cystic duct. The cystic duct connects with the common hepatic duct to form the common bile duct. The common bile duct eventually joins with the main pancreatic duct to empty into the duodenum via the sphincter of Oddi.
The biliary system refers to the organs (liver and gallbladder) and ducts (hepatic, cystic and common bile ducts) that secrete or store, and empty bile into the duodenum.
Bile is continuously produced by the liver. The gallbladder serves to store and concentrate bile between periods of digestion. The presence of chyme in the duodenum triggers the release of cholecystokinin (CCK)* from the duodenal mucosa. CCK causes contraction of the gallbladder and a relaxation of the sphincter of Oddi, allowing bile to be released into the duodenum.
Lower GI Tract
The lower GI tract contains the following structures:
-
-
- small intestine
- large intestine
- rectum
- anus
-
We’ll discuss each of these in more detail.
Small Intestine
The small intestine is the portion of the gastrointestinal tract that begins at the pyloric sphincter of the stomach and ends at the ileocecal junction*, the start of the large intestine (colon).
The small intestine is a coiled 6 to 7 metre (approximately 20 feet) long tube and consists of three parts:
-
-
- duodenum
- jejunum
- ileum
-
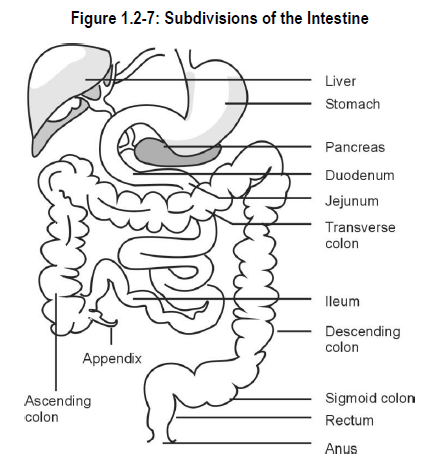
See Figure 1.2-7.
The duodenum is the shortest, widest and most fixed segment of the small intestine and is approximately 25 centimetres (10 inches) in length. Its shape is generally that of a horseshoe. The opening of the common bile duct is found about halfway down the length of the duodenum.
The remainder of the small intestine is about 6 metres (20 feet) in length. Its proximal two fifths are customarily referred to as the jejunum and its distal three fifths as the ileum. There is no sharp division between the jejunum and ileum. Most digestion occurs in the jejunum and ileum.
The major function of the small intestine is absorption of dietary components, endogenous* compounds (e.g., bile salts) and most drugs.
Large Intestine (Colon)
The large intestine (colon) is 1.4 to 1.7 metres (4-5 feet) in length. Its diameter is greatest proximally and narrows distally.
The large bowel can be divided into the following sections:
-
-
- the cecum
- the ascending colon
- the transverse colon
- the descending colon
- the sigmoid colon
-
See Figure 1.2-8.
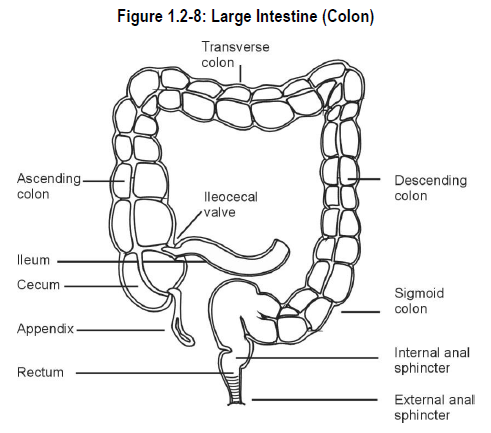
The primary function of the large intestine is the concentration (by removal of water) and storage of intestinal wastes.
The large intestine participates in an important way in the maintenance of water and electrolyte balance in the body by exchanging considerable amounts of salts across its membranes and returning water to the circulation. As water is reabsorbed from the large intestine back into the body, the liquid waste in the intestine is converted into solid material.
Microorganisms present in the large intestine synthesize some vitamins and produce gas (flatus).
1) Cecum
The entrance to the cecum is controlled by the ileocecal valve that prevents significant reflux of colonic contents back into the small intestine.
2) Appendix
The appendix is a worm-like, dead-end tube approximately 8.5 centimetres (approximately 3 inches) in length that hangs off the cecum. It is considered an embryonic remnant with no known function.
A number of physiological events may occur which may lead to inflammation or occlusion and subsequent necrosis of the appendix. Appendicitis* is the most common reason for emergency abdominal surgery.
3) Ascending Colon
The ascending colon is the vertical section of the large intestine that is found on the right side of the abdominal cavity. It extends upward from the cecum to just under the liver.
4) Transverse Colon
The transverse colon is the horizontal section of the colon in the upper part of the abdominal cavity.
5) Descending Colon
The descending colon is the vertical section of the large intestine that is found on the left side of the abdominal cavity, and extends down toward the rectum to the pelvic brim
6) Sigmoid Colon
The sigmoid colon is an S-shaped section of the large intestine distal to the descending colon and connects the colon to the rectum
Rectum
Beyond the sigmoid colon, the bowel once again dilates to form the rectum. The rectum is that portion of the large bowel interposed between the terminal portion of the sigmoid colon and the anal canal. See Figure 1.2-8.
When a sufficient mass of waste products including undigested and indigestible material reaches the rectum it is expelled from the body through the anal opening. This mass of expelled waste products is referred to as feces or stool.
Anus (Anal Canal)
The anus or anal canal (the exit from the rectum) makes up the terminal 3 centimetres of the gastrointestinal tract and arises from a tissue of different origin than that of the rectum.
Both the rectum and anal canal are surrounded by muscular tissue.
Anal sphincter muscle contraction maintains closure of the rectum until the act of defecation, when contraction of muscle in the rectum and anal canal aids in the clearance of fecal material.
There are two anal sphincters:
-
-
- the internal anal sphincter
- the external anal sphincter
-
The external anal sphincter is under voluntary control allowing defecation to be delayed if necessary.
SECTION 2B: Glandular Secretions
Saliva
Saliva is secreted by three pairs of salivary glands:
-
-
- parotid glands
- sublingual glands
- submandibular glands
-
See Figure 1.2-10.
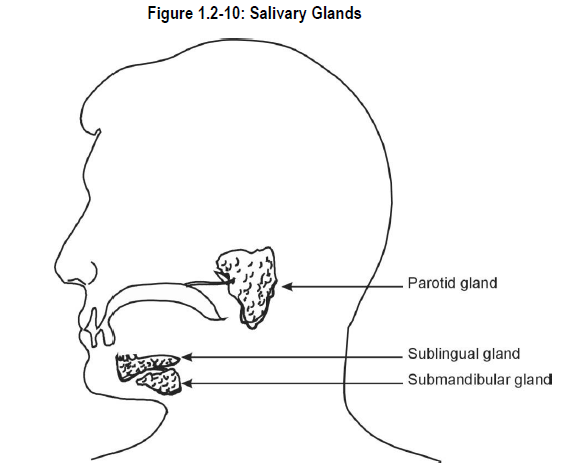
Saliva is a mixture of mucus and watery fluid containing digestive enzymes.
Important functions of saliva include:
-
-
- moistening and lubricating food prior to swallowing
- beginning starch digestion by amylase contained in saliva
- dissolving food molecules which can then be tasted by the
- chemoreceptors* in the mouth
-
Gastric Secretion Phases
Within the stomach, food is broken down by the chemical action of gastric secretions and physically by the action of the stomach musculature.
Gastric secretions (acids and enzymes) aid in the chemical breakdown of food into a semifluid substance called chyme, which can be passed to the small intestine for further digestion and absorption. Two to three litres of gastric secretions are produced daily. Both neural and hormonal* factors regulate the secretion of gastric juice. There are three phases of gastric secretion:
-
-
- Cephalic* phase – The cephalic phase of gastric secretion occurs in response to the sight and smell of food and to chewing or the presence of food in the mouth. This stimulates the parasympathetic nervous system* reflexes to increase the production and release of gastric secretions.
- Gastric phase – The gastric phase of secretion is initiated by the stretching of the stomach due to the presence of food and by the breakdown products of protein digestion. This stimulates the release of the stomach hormone gastrin*, which stimulates the stomach to produce more gastric juice.
- Intestinal phase – The intestinal phase of gastric secretion produces an inhibitory effect on gastric secretion, and is brought about by the presence of digested food (chyme) in the small intestine.
-
Thousands of specialized gastric secretory cells are found in the stomach lining and in digestive glands that are buried within the mucosa (in pits). These are the cells that secrete gastric juice containing digestive enzymes and hydrochloric acid (HCl) into the stomach.
Gastric Digestive Glands
1) Gastric glands
Two major types of gastric glands (Oxytin and Pyloric glands) are responsible for gastric secretions and are located in the fundus and body of the stomach These glands contain the following types of secretory cells
-
-
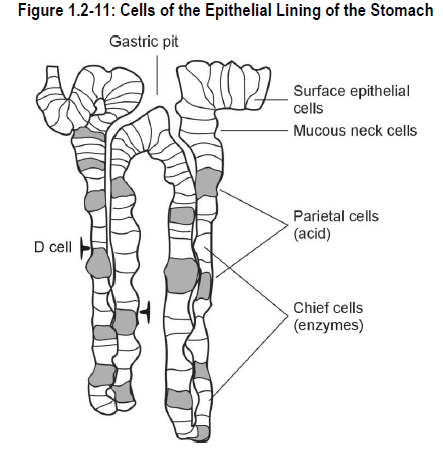
- the parietal cells* – secrete hydrochloric acid and
- intrinsic factor*
- the chief cells* (also called zymogenic cells*) – secrete pepsinogen*, the precursor for pepsin
- the mucous neck cells* – secrete a sticky mucus to protect the stomach wall from being damaged by its own acid and digestive enzyme secretions (See Figure 1.2-11)
- D cells* – secrete somatostatin, which is a regulatory peptide
-
2) Pyloric (antral) glands
The pyloric glands are located in the antrum and pyloric regions of the stomach and contain two types of secretory cells:
-
-
- the G cells* which release the hormone gastrin
- mucous cells which secrete mucus
-
Gastric Secretions
1) Hydrochloric Acid
Hydrochloric acid performs the following functions:
-
-
- breaks down protein
- provides an optimal pH for the action of pepsin
- prevents the growth of bacteria from ingested food
-
The fasting stomach continuously secretes acid. Peak amounts are released near midnight and lowest quantities shortly before awakening.
Histamine* receptors in the stomach are called H2 receptors. Activation of H2 receptors on the parietal cells of the stomach stimulates HCl secretion. The formation and secretion of gastric acid occurs in two stages.
In the first stage, histamine, acetylcholine* (secreted by the vagus nerve*), or gastrin stimulate their respective receptor on parietal cells to begin the process of acid formation.
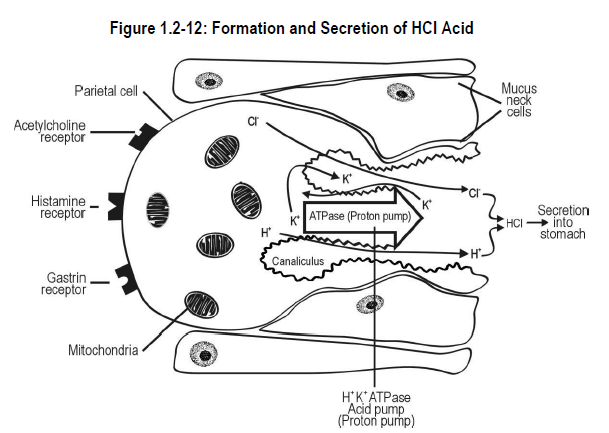
In the second stage, the enzyme H+K+ATPase* (often called the proton pump) completes the formation and secretion of gastric acid.
The steps involved in this process are:
-
-
- transport of potassium ions (K+) and chloride ions (Cl-) into the parietal cell canaliculus*
- exchange of hydrogen ion (H+) for K+ by the ATPase active transport system* (or H+K+ATPase pump)
- resultant formation of HCl and secretion into the stomach
-
The proton pump is the final common pathway for the secretion of gastric acid.
Numerous mitochondria* provide energy for the active transport process. See Figure 1.2-12.
2) Intrinsic Factor
Intrinsic factor, secreted by parietal cells, is required for the absorption of vitamin B12.
Intrinsic factor forms a complex with vitamin B12 and this complex is carried to the small intestine where the vitamin is absorbed.
3) Gastrin
The primary functions of gastrin, the hormone secreted by the G cells, include:
-
-
- stimulation of the parietal cells to secrete HCl
- increasing gastrointestinal motility
- increasing pancreatic secretions
-
4) Pepsinogen
Pepsinogen, secreted by the chief cells in the stomach, is converted to its active form pepsin.
Pepsin is a proteolytic enzyme that begins the process of protein digestion.
5) Other gastric secretions
Somatostatin* is a regulatory peptide produced by D cells of the gastric mucosa. Somatostatin inhibits the release of gastrin from the G cells of the stomach. Somatostatin also inhibits the release of pancreatic secretions.
Prostaglandins are also produced by the surface cells of the stomach. Prostaglandins have a protective effect on the lining of the stomach and duodenum against ulceration. Certain drugs (e.g., nonsteroidal anti-inflammatory drugs or NSAIDs*) block the production of prostaglandins and increase the risk of gastrointestinal ulceration.
Pancreatic Enzymes
The exocrine cells of the pancreas produce four types of digestive enzymes:
-
-
- peptidases (trypsin, chymotrypsin and carboxypeptidases) – digest proteins
- lipases – digest fats
- amylases – digest carbohydrates (starches)
- nucleases (ribonuclease, deoxyribonuclease) – digest nucleic acids
-
The release of pancreatic secretions is stimulated by the vagus nerve and local hormones. The presence of chyme in the duodenum stimulates the duodenal mucosa to produce several hormones including:
-
-
- secretin* – primary effect is to increase bicarbonate ion secretion by the pancreas
- cholecystokinin (CCK) – hormone that provides the major stimulus for the secretion of pancreatic enzymes
-
Both CCK and secretin are referred to as enterogastrones. Enterogastrones are intestinal hormones. Both CCK and secretin, while stimulating the pancreas, have inhibiting effects on gastric smooth muscle.
Bile
Bile is produced by hepatocytes* at the rate of about 1 litre per day.
Bile has two primary functions. Bile is:
-
-
- required for the digestion and absorption of fats and fat soluble vitamins (A,D,E and K)
- an excretory medium for water-insoluble substances such as cholesterol and bilirubin and other waste products produced by the liver
-
Bilirubin, the main bile pigment formed in the liver, is a breakdown product of hemoglobin. Bile pigments are responsible for the yellow colour of bile and the brown colour of stool.
Secretions of the Small Intestine
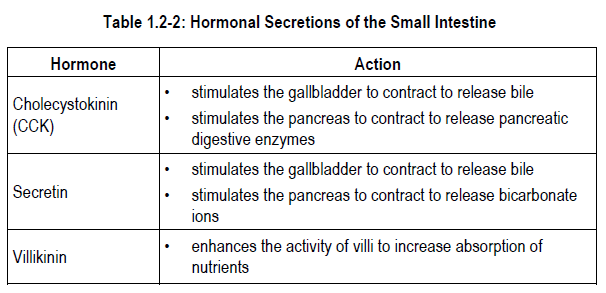
The mucosa of the small intestine also produces a number of hormones that control functions of the pancreas, gallbladder and intestine.
As previously discussed, the hormones secretin and CCK stimulate contraction of the gallbladder to release bile. In the pancreas, secretin stimulates the release of bicarbonate ions; CCK stimulates the release of pancreatic digestive enzymes.
Villikinin* is another intestinal hormone. The function of villikinin is the stimulation of movement of the intestinal villi* to enhance the absorption of nutrients.
Large quantities of mucus are also produced by glands in the mucosal wall of the small intestine and, as in the stomach, the mucus serves to protect the GI tract wall from the acidic chyme.

SECTION 2C: Motility along the GI Tract
Swallowing
Swallowing is a complex process that requires the co-ordinated activity of a number of GI structures. See Figure 1.2-13a.
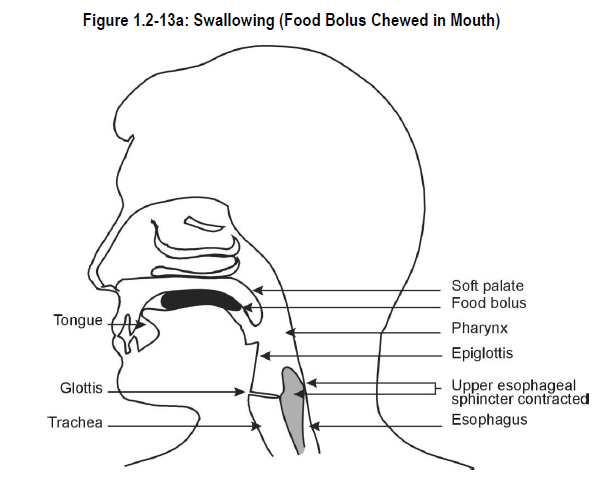
Chewed food is pushed back and against the soft palate by the tongue. This forces the soft palate to rise, blocking the nasal passages as the chewed food enters the pharynx.
Since the pharynx serves as a common passageway for both air from the nose and food from the mouth, there are mechanisms in place to prevent food from entering the respiratory tract (trachea*). These mechanisms include:
-
-
- inhibition of respiration during swallowing
- raising of the soft upper palate to block off the nasal airway
- closure of the glottis* and vocal chords
- lowering of the epiglottis*, by the movement of the food, to cover the larynx and trachea
- opening of the upper esophageal sphincter
-
See Figure 1.2-13b.
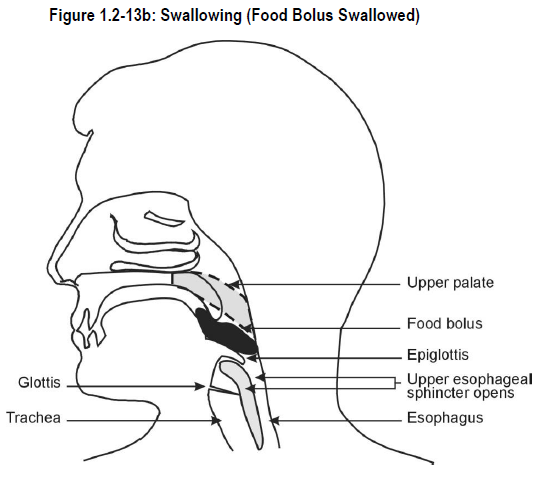
Contractions of the pharyngeal muscles push food into the esophagus and the upper esophageal sphincter contracts. See Figure 1.2-13c.
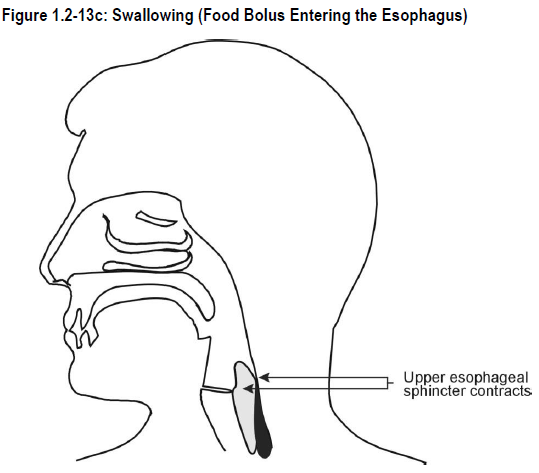
Esophagus
As mentioned previously, the esophageal sphincters keep the esophagus closed except during the act of swallowing.
The esophagus is supplied by both parasympathetic and sympathetic* innervation and is subject to both voluntary and involuntary nervous control. The vagus nerve is the major parasympathetic tract that innervates the esophagus.
The normal muscular activity of the esophagus and its upper and lower sphincters is dependent upon a series of highly complicated stimulatory and inhibitory reflex neural actions.
Gastric Motility
The muscularis of the stomach wall, in addition to the circular and longitudinal muscle layers, contains a third obliquely arranged layer of muscle. This additional muscle layer contributes to the stomach’s ability to churn, mix and break down ingested food.
Approximately every 20 seconds, mixing waves move through the muscularis of the stomach to aid in mixing the food with gastric secretions until semifluid chyme is produced.
Gastric peristaltic waves occur at the rate of about 3 per minute and are generated by pacemaker cells in the longitudinal muscle layer. These spontaneous depolarization-repolarization cycles are referred to as the basic electrical rhythm of the stomach.
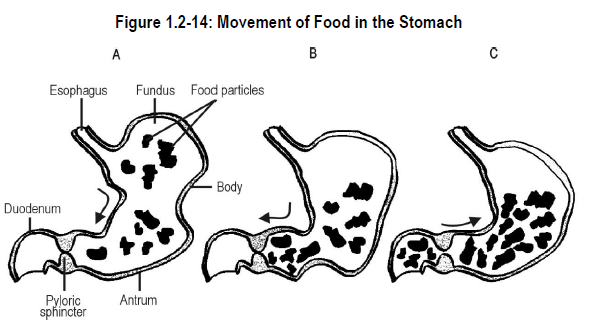
Figure 1.2-14 depicts the movement of food in the stomach. The gastric peristaltic waves force the chyme towards the pylorus of the stomach and, at the same time, cause the closure of the pyloric sphincter, the connection between the pylorus and duodenum. See Figure 1.2-14 A and B.
Since the pyloric sphincter closes as a peristaltic wave approaches, only a small amount of chyme is allowed to enter the duodenum with each peristaltic wave. The rest of the chyme is forced backward into the body of the stomach for more mixing. See Figure 1.2-14 C.
Between periods of digestion, any food left in the stomach is removed by the migrating motor complex (MMC). The MMC is a peristaltic wave that begins in the esophagus and moves the entire length of the GI tract approximately every 60-90 minutes.
Motilin*, a hormone released from the epithelium of the small intestine, increases the strength of the MMC.
Intestinal Motility
The small intestine undergoes two motion patterns:
-
-
- peristalsis (as previously described)
- segmentation
-
During a meal, small sections of the intestine contract and relax in a rhythmical pattern, with minimal forward movement of the chyme along the bowel. This motion is referred to as segmentation.
Segmentation chops and mixes the chyme to facilitate its exposure to the intestinal villi thereby improving nutrient absorption.
Anal Sphincter
As described previously, anal sphincter muscle contraction maintains closure of the rectum until the act of defecation, when contraction of muscle in the rectum and anal canal aids in the clearance of fecal material.
SECTION 2D: Absorption of Nutrients
Stomach
Minimal absorption of nutrients takes place in the stomach.
Small Intestine
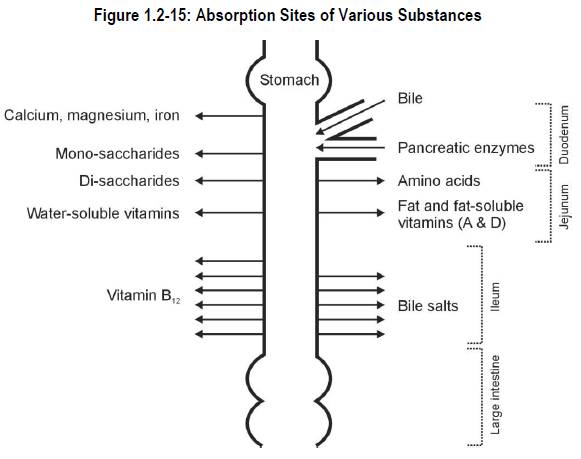
As mentioned previously, the major function of the small intestine is absorption of dietary components, endogenous compounds (e.g. bile salts) and most drugs. The absorption site of certain compounds is depicted in Figure 1.2-15.
Simple sugars, amino acids, fat, vitamins and minerals are absorbed into the blood vessels of the submucosa. The absorption process is accomplished by active transport. Active transport means that energy is required to move each molecule through the membrane.
Mitochondria, specialized cell components in which energy-producing chemical changes occur, supply the energy for this process.
The wall of the small intestine is not permeable to large molecules. Absorption does not occur if nutrients are not broken down sufficiently or if the mitochondria are unable to produce sufficient energy for the active transport process.
Villi and Microvilli
The mucosa of the small intestine is modified to allow for the absorption of nutrients.
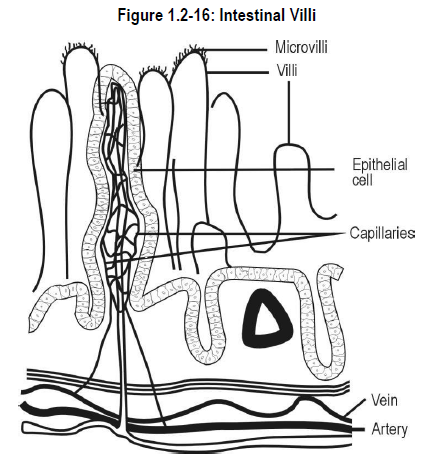
The mucous membrane of the small intestine is composed of a single layer of columnar epithelial cells. Protruding from the surface of the mucous membrane are multiple finger-like projections known as villi (see Figure 1.2-16).
From the surface of each villus are even smaller projections called microvilli* (sometimes referred to as the brush border).
Villi and microvilli increase the absorptive surface of the small intestine several hundred-fold and their presence causes the mucosal surface to appear velvety.
SUMMARY — SECTION 2: Anatomy and Physiology
Our GI system converts food into molecular forms that can be absorbed and used for tissue building, repair and energy.
In the mouth, food is chewed, mixed with saliva secreted by the salivary glands and then swallowed. Peristaltic contractions of the pharynx push food into the esophagus. The esophagus moves the food or fluid from the pharynx into the stomach by peristalsis. The esophagus possesses no significant secretory or absorptive functions.
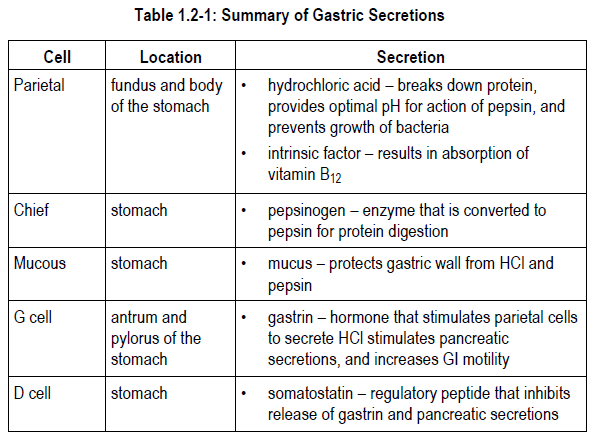
The stomach stores food, mixes food with gastric secretions to form chyme, and regulates the delivery of the chyme to the small intestine. Minimal absorption takes place in the stomach. The gastric mucosa protects the stomach against gastric secretions and against noxious agents present in ingested material. The secretions are released by gastric glands and pyloric glands and include:
-
-
- hydrochloric acid – breaks down protein, provides optimal pH for action of pepsin, and prevents growth of bacteria
- intrinsic factor – results in absorption of vitamin B12
- pepsinogen – enzyme that is converted to pepsin for protein digestion
- mucus – protects gastric wall from HCl and pepsin
- gastrin – hormone that stimulates parietal cells to secrete HCl, stimulates pancreatic secretions and increases GI motility
- somatostatin – regulatory peptide that inhibits release of gastrin and pancreatic secretions
-
Muscle layers contribute to the stomach’s ability to churn, mix and break down ingested food. Mixing waves that move through the muscularis of the stomach aid in mixing the food with gastric secretions. Gastric peristaltic waves force the chyme towards the duodenum. Between periods of digestion, any food left in the stomach is removed by the migrating motor complex (MMC). The hormone motilin increases the strength of the MMC.
The walls of the GI tract have a similar basic structure, which is modified along the tract for special functions. All the layers of the GI tract wall contain networks of nerve fibres that are part of the autonomic nervous system.
The pancreas secretes enzymes that digest fats, proteins and carbohydrates into simpler substances and bicarbonate ions that neutralize the highly acidic chyme from the stomach.
The liver performs many metabolic and regulatory functions. The primary digestive function of the liver is the production and secretion of bile. In the liver, the hepatic portal vein receives blood from the intestinal tract, which allows the liver the first chance to process nutrients and drugs from the blood stream after the blood leaves the intestine. This is called the first-pass effect.
Bile is stored in the gallbladder. The gallbladder contracts intermittently during meals to release bile into the duodenum. Bile is required for the digestion and absorption of fats and fat soluble vitamins (A, D, E and K). It is also an excretory medium for cholesterol and bilirubin and other waste products produced by the liver.
The small intestine consists of the duodenum, jejunum, and ileum. The major function of the small intestine is absorption of dietary components, endogenous compounds (e.g. bile salts) and most drugs through the villi and microvilli. Simple sugars, amino acids, fat, vitamins and minerals are absorbed by active transport into the blood vessels of the intestinal submucosa.
The following hormones are released from the intestinal mucosa:
-
-
- cholecystokinin (CCK) — stimulates the gallbladder to contract to release bile and the pancreas to contract to release pancreatic digestive enzymes
- secretin — stimulates the gallbladder to contract to release bile and the pancreas to contract to release bicarbonate ions
- villikinin — enhances the activity of villi to increase absorption of nutrients
-
Peristalsis and segmentation aid in the movement of material in the small intestine. Segmentation increases the exposure of the chyme to the intestinal villi.
The primary function of the large intestine, also called the colon, is the concentration and storage of intestinal wastes. Microorganisms present in the large intestine synthesize some vitamins and produce gas (flatus).
When a sufficient mass of waste products including undigested and indigestible material reaches the rectum it is expelled from the body through the anal opening.
PROGRESS CHECK — SECTION 2: Anatomy and Physiology
1.
Mastication is another term for the act of _________________________ .
2.
Indicate whether each of the following is true or false.

3.
The stomach performs three main functions which include the storage of food after a meal, the mixture of food with gastric secretions and
_________________________
4.
Indicate whether each of the following is true or false.

5.
In addition to moistening food and beginning the process of digestion, saliva also
_________________________
_________________________
6.
The _________________________ is the final common pathway for the secretion of gastric acid.
7.
Complete the following table by stating the function of the gastric secretions.
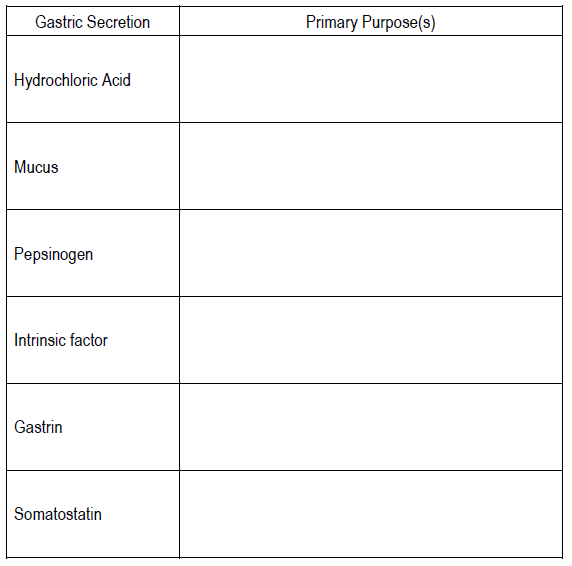
8.
The pancreas secretes both _________________________ and _________________________ that are important in the digestive process.
9.
Bile is required to aid in the digestion of _________________________ .
10.
Two hormones secreted by the duodenal mucosa are _________________________ and _________________________.
11.
HCl is produced by the _________________________ cells of the stomach.
12.
The _________________________ covers the top of the trachea during the act of swallowing.
13.
The strength of the migrating motor complex is increased by _________________________ .
14.
The absorption surface of the small intestine is increased by the presence of _________________________ and _________________________.
PROGRESS CHECK ANSWERS — SECTION 2: Anatomy and Physiology
1.
Mastication is another term for the act of chewing.
2.
1) False
The esophagus propels food from the pharynx into the stomach by a process called peristalsis.
2) True
3) True
4) True
3.
the regulation of the delivery of chyme to the small intestine
4.
1) False
The small intestine contains the duodenum, jejunum and ileum.
2) False
The primary function of the small intestine is the absorption of nutrients. Water is absorbed in the large intestine.
3) True
4) True
5.
dissolves some of the food chemicals so they can be tasted by chemoreceptors in the mouth
6.
The proton pump is the final common pathway for the secretion of gastric acid.
7.
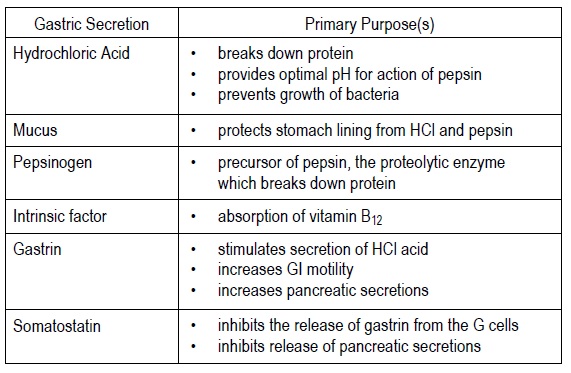
8.
The pancreas secretes both digestive enzymes and bicarbonate ions that are important in the digestive process.
9.
Bile is required to aid in the digestion of fats.
10.
Two hormones secreted by the duodenal mucosa are cholecystokinin (CCK) and secretin.
11.
HCl is produced by the parietal cells of the stomach.
12.
The epiglottis covers the top of the trachea during the act of swallowing.
13.
The strength of the migrating motor complex is increased by motilin.
14.
The absorption surface of the small intestine is increased by the presence of villi and microvilli.
MODULE 1 Test
1.
The primary function of the GI system is to:
a) produce and release hormones
b) break down food
c) remove wastes from the body
2.
Which of the following is a glandular organ associated with the GI system?
a) liver
b) pharynx
c) esophagus
d) colon
3.
Which of the following statements is true?
a) the esophagus connects the stomach to the large intestine
b) the esophagus secretes enzymatic juices that aid digestion of food
c) the gastroesophageal sphincter prevents gastric contents from flowing back into the esophagus
d) the gastroesophageal sphincter is a sac-like structure connected to the bottom of the esophagus
4.
All of the following are anatomical subdivisions of the stomach EXCEPT:
a) cardia
b) ileum
c) fundus
d) antrum
5.
The pancreas:
a) aids in the breakdown of bilirubin
b) secretes enzymes that digest fats, protein and carbohydrates
c) secretes bile
d) receives blood from the hepatic portal vein
6.
Which of the following are anatomical subdivisions of the small intestine?
a) ascending colon, transverse colon, descending colon and sigmoid colon
b) pylorus, duodenum, pancreas, gallbladder and cecum
c) duodenum, ileum, cecum and rectum
d) duodenum, jejunum and ileum
7.
Bile is stored in the:
a) liver
b) gallbladder
c) pancreas
d) small intestine
8.
The primary role of the large intestine is to:
a) secrete the hormone secretin
b) absorb nutrients
c) remove water from wastes
d) expel indigestible material from the body
9.
HCl secretion is stimulated by:
a) intrinsic factor
b) pepsinogen
c) somatostatin
d) gastrin
10.
Enzymes involved in fat digestion are called:
a) lipases
b) peptidases
c) amylases
d) nucleases
MODULE 1 Test Answers
1.
b) break down food
2.
a) liver
3.
c) the gastroesophageal sphincter prevents gastric contents from flowing back into the esophagus
4.
b) ileum
5.
b) secretes enzymes that digest fats, protein and carbohydrates
6.
d) duodenum, jejunum, and ileum
7.
b) gallbladder
8.
c) remove water from wastes
9.
d) gastrin
10.
a) lipases
