Module 1: Gerontology
Introduction
Aging is a normal process. As we age, our bodies begin to decline. This decline takes place at a faster rate in some people compared to others, and may result in a greater degree of disability.
In this module, we focus on the effects of aging on the body’s organs, how drug dosing is affected in the elderly, and the demographics of Canada’s elderly population.
Module Structure
This module contains 3 sections:
Section 1: Aging
Section 2: Drug Dosing in the Elderly
Section 3: Demographics
Section 1: Aging
After reading this section, you should be able to:
- Define the terms aging and senior.
- Explain the causes of aging.
- Explain the main effects of aging on the body systems.
- Identify common disorders that are associated with aging.
Description of Aging
Aging is a normal process that takes place gradually throughout the lifespan. Aging occurs as a result of a complex combination of normal physiologic changes and the effects of comorbid illnesses. While some diseases are more common in older people, diseases are not a normal part of aging. Through healthy lifestyle choices, some people are able to slow down, or even avoid, many of these diseases.
The average life expectancy of Canadians has been increasing but the maximum age reached has not changed a great deal over the years. The maximum life span is approximately 125 years for women and a bit shorter for men.
No specific age defines a person as being elderly. When we refer to a person as being elderly or a senior, we are generally referring to a person aged 65 or older. With regards to a person’s state of health, chronological age is a less important contributing factor than the presence and severity of comorbid illness. There is broad heterogeneity of health, mental and functional status among seniors.
Causes of Aging
The exact cause of aging is not known.
A person’s genetic make-up plays a key role in determining how long cells live and the rate at which a person ages. Cells continually undergo many chemical reactions during which toxins may be released. These toxins or free radicals damage cells, thus contributing to aging of the cells.
Healthy lifestyle choices such as adhering to a healthy diet, maintaining a healthy weight, exercising regularly, and not smoking cigarettes are important determinants in aging successfully. Exposure to toxins in the environment or workplace may affect the function of the kidneys, lungs, liver and nervous system.
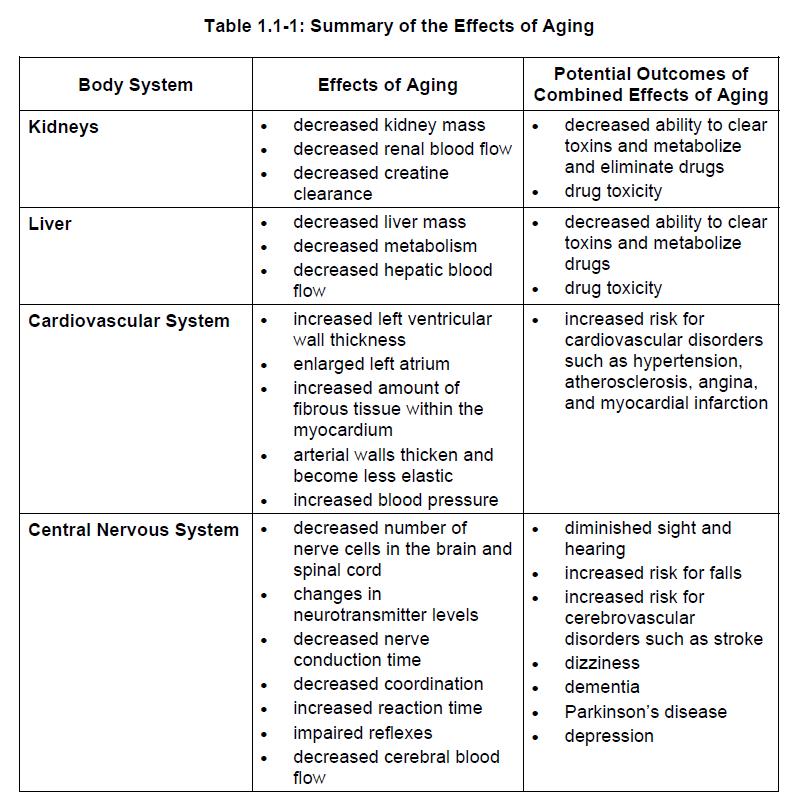
Effects of Aging
With advancing age, the body’s composition changes. The lean body mass decreases, bone and body organ mass may decrease slightly, and water volume decreases. The proportion of body fat increases and the distribution of fat changes, with more fat being present in the abdominal area and less fat under the skin.
With aging, kidney mass decreases. Renal blood flow decreases significantly, resulting in decreased creatine clearance. Liver mass also decreases resulting in decreased metabolism and decreased hepatic blood flow. These changes in the liver and kidney affect the ability of a senior to clear toxins and metabolize drugs. We discuss drug dosing in the elderly in more detail in Section 2.
Changes also take place in other organs of the body as a person ages. These changes may contribute to diseases in the elderly. Several disorders occur only in older adults. Some disorders may be more common or more severe in seniors, or may present with different symptoms.
1) Cardiovascular system
With normal aging, the left ventricular wall thickens slightly. The left ventricular cavity and the left atrium may also increase slightly in size. Arterial walls become thicker and less elastic.
Heart rate decreases slightly from age 20 to age 80 in healthy men and women. Cardiac output decreases slightly in older women but is not reduced in older men.
These changes in the cardiovascular system place elderly patients at increased risk for cardiovascular disorders such as hypertension*, atherosclerosis*, angina*, and myocardial infarction*. Heart failure occurs when the heart is unable to deliver an adequate supply of blood to the body. We discuss cardiovascular disorders in more detail in Module 2.
2) Nervous system
The number of functioning neurons in the brain decreases with age. There may also be a decrease in the number of neurotransmitters and receptors. This could lead to decreased levels of serotonin*, catecholamine* and acetylcholine and increased monoamine oxidase* levels.
The resulting disorders include diminished sight and hearing, increased risk for falls, or increased risk for cerebrovascular disorders such as stroke*.
Aging may also affect cognition, memory, intelligence, personality and behaviour, leading to disorders such as Parkinson’s disease*, Alzheimer’s disease*, or depression*.
We discuss disorders of the nervous system in more detail in Module 3.
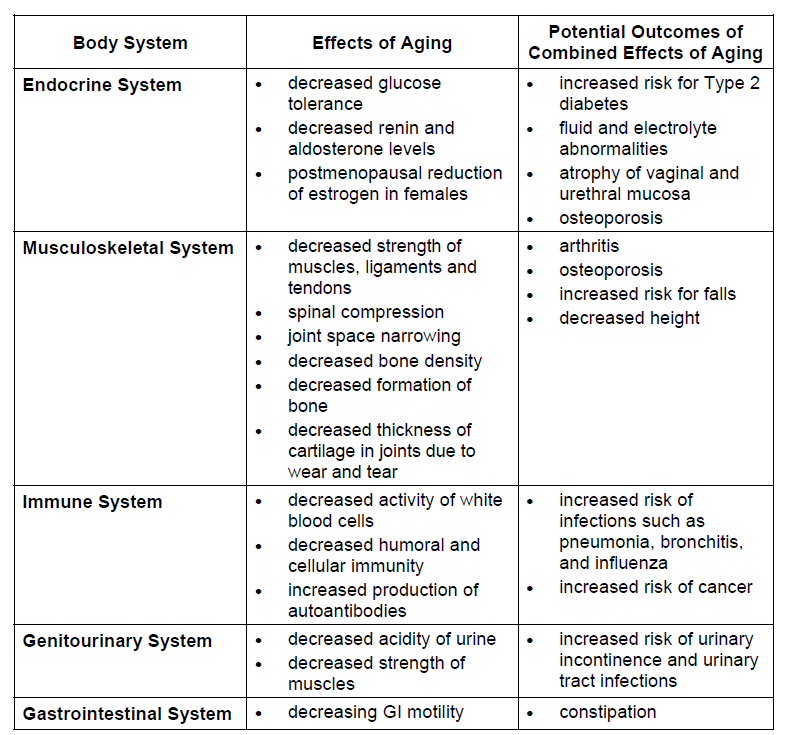
3) Endocrine system
Many elderly persons have altered carbohydrate metabolism and changes in glucose tolerance with aging. Fasting glucose and post-prandial plasma glucose levels both increase after age 30 to 40. This means that the elderly are at increased risk of developing Type 2 diabetes*. Type 2 diabetes is discussed in more detail in Module 4.
The renin-angiotensin-aldosterone system is also affected by aging. Lower renin*, aldosterone*, and angiotensin II* levels in the elderly contribute to fluid and electrolyte abnormalities and may also contribute to dehydration.
Postmenopausal females are at increased risk of various disorders (e.g., osteoporosis*, cardiovascular disease, atrophy* of vaginal and urethral mucosa) due to decreased estrogen levels.
4) Musculoskeletal system
Bone density starts to decrease in both men and women after age 30, but decreases more rapidly in women in the years immediately post menopause due to decreased levels of estrogen. Decreased bone density may result in osteoporosis accompanied by an increased risk of fractures due to fragile bones.
Other changes that occur with age include:
-
-
- decreased formation of bone and increased resorption or breakdown of bone
- decreased thickness of cartilage in joints due to wear and tear
- decreased strength of ligaments and tendons
-
We discuss osteoarthritis* and osteoporosis in more detail in Module 5.
5) Immune system
With advancing age, the activity of white blood cells (e.g., T-lymphocytes, neutrophils) involved in nonspecific response of the body to invading microorganisms and the immune system decreases. Humoral immunity (B-lymphocyte mediated), which involves the production of antibodies that can eliminate harmful antigens, also decreases with age. Cellular immunity (T-lymphocyte mediated) decreases and results in delayed hypersensitivity reactions*.
Respiratory tract infections such as pneumonia* and bronchitis* are more prevalent in the elderly. The loss of elastic tissue and weakened musculature in the lower airways decrease the ability to cough up secretions. Mucociliary transport of secretions and foreign material is also decreased. These changes result in increased opportunities for invasion by microorganisms.
Decreased acidity of urine and incomplete emptying of the bladder place elderly persons at increased risk of urinary tract infections.
We discuss infectious diseases in more detail in Module 6 and cancer in Module 7.
6) Genitourinary system
Bladder capacity, contractility and the ability to postpone voiding decline with age. In women, the urethra shortens and the strength of the urethral sphincter declines. In men, the size of the prostate gland increases. All of these changes in the urinary tract place the elderly at increased risk of developing a genitourinary disorder. We discuss genitourinary disorders in more detail in Module 8.
7) Gastrointestinal system
Aging is also accompanied by slower metabolism and decreasing gastrointestinal motility, which may lead to constipation.
As we age, our ability to absorb nutrients declines and our metabolism slows. Elderly people tend to feel fuller sooner with less food. However, if the intake of adequate nutrients does not meet the body’s requirements, malnutrition may occur. We discuss malnutrition in more detail in Module 9.
Summary — Section 1: Aging
A senior is generally someone who is 65 years of age or older. Many of today’s seniors are living longer and many remain healthier into their later years compared to seniors of previous generations.
Although the aging process is normal and gradual, normal aging may be accompanied with a variety of diseases and disorders. Some people are able to slow down, or even avoid, many of the diseases common to the elderly by adhering to a healthy lifestyle.
The exact cause of aging is not known but genetics and lifestyle are important determinants as to how long a person lives and whether or not they are at risk for diseases of the elderly.
With advancing age, the body’s composition changes and several changes in the body’s organs gradually occur. These changes mean that seniors have a decreased ability to clear toxins and metabolize and eliminate drugs. Seniors are also at increased risk for a variety of diseases and disorders such as:
-
-
- cardiovascular disorders such as hypertension, atherosclerosis, angina, and myocardial infarction
- central nervous system disorders such as dementia, Parkinson’s disease, depression, and stroke
- Type 2 diabetes
- arthritis
- osteoporosis
- infections such as pneumonia, bronchitis, influenza and urinary tract infections
- cancer
- urinary incontinence
- constipation
-
Progress Check — Section 1: Aging
1.
Indicate whether each of the following statements is True or False.

2.
What is the effect of aging on the kidneys?
____________________________________
____________________________________
____________________________________
____________________________________
3.
What is the effect of aging on the liver?
___________________________________
___________________________________
___________________________________
___________________________________
4.
Seniors are at increased risk for Type 2 diabetes due to decreased _______________.
Progress Check Answers — Section 1: Aging
1.
1) True
2) False
Senior generally refers to those people who are age 65 or older.
3) True
2.
The following are effects of aging on the kidney:
-
-
- kidney mass decreases
- renal blood flow decreases significantly
- creatine clearance decreases
-
3.
With aging, the liver mass decreases resulting in:
-
-
- decreased metabolism
- decreased hepatic blood flow
-
4.
glucose tolerance
Section 2: Drug Dosing in the Elderly
Learning Objectives
After reviewing this section, you should be able to:
- Describe the impact of age-related changes in pharmacokinetics on drug response in the elderly.
- Discuss the effects of liver and/or kidney disease on the absorption, distribution and elimination of drugs.
- Describe the impact of age-related changes in pharmacodynamics on drug response in the elderly.
- Explain why the elderly are at risk of polypharmacy.
- Explain why compliance may be an issue with the elderly.
Pharmacotherapy in the Elderly
Since the elderly patient is often taking multiple medications for concomitant disorders, this group requires special consideration. With the exception of most antibiotics, the approach to selecting a dose of a drug for an elderly patient should be to start with a low dose and titrate upward slowly as tolerated.
The risks of adverse reactions associated with medications are greater in an older population due to:
-
-
- changes in pharmacokinetics and pharmacodynamics associated with aging
- increased vascular, renal and neurological disorders
- multiple medications
-
Compliance is also a concern. It is important that patients understand the need for their medication and dosing requirements.
Pharmacokinetic Changes in the Elderly
The pharmacokinetic consequences of aging include changes in absorption, distribution, and metabolism and excretion of medications.
1) Absorption
Changes take place in the gastrointestinal tract with advancing age, but its anatomic and physiologic integrity is generally well maintained. Changes that may theoretically alter drug absorption include decreased acid secretion in the stomach, decreased gastric motility and reduced first-pass metabolism.
-
-
- decreased acid secretion
An increase in gastric pH due to reduced acid secretion occurs much more frequently in older patients and causes the ratio of nonionized/ionized molecules of weakly acidic drugs to decrease. This may reduce the extent of absorption of drugs from the stomach that require acid for absorption (e.g., fluconazole). Achlorhydria* occurs rarely, but would enhance this effect. - decreased gastric motility
Delayed gastric emptying has the effect of delaying the onset of action since the drug is released more slowly to the duodenum and small intestine where the majority of absorption occurs. Absorption of drugs usually remains unchanged in the elderly despite increased gastric pH and decreased GI motility. - decreased first-pass effect
The bioavailability of some drugs with a high rate of first-pass metabolism (e.g., propranolol) may be increased, because of decreased first-pass extraction common to the elderly.
- decreased acid secretion
-
2) Drug distribution
-
-
- volume of distribution
Volume of distribution (Vd) is a mathematical concept. It is the justification for a given serum concentration after administering a dose of a drug. If the dose administered produces a low serum concentration, then the Vd is large.Both body weight and body composition change with advancing age. Intracellular water decreases from 42% to 33% and fat content increases from 15% of body weight to 30% of body weight when the average 25-year-old is compared to the average 75-year-old.These changes in body composition have effects on the drug concentration achieved, depending on whether the drug is water-soluble or fat-soluble. For drugs that distribute into body water (e.g., digoxin, lithium, aminoglycoside antibiotics), the reduction in body water with aging will result in a smaller Vd and a higher serum drug concentration after a typical dose of the drug. A lower initial dose may be required in the elderly to avoid drug toxicity.For drugs that distribute into body fat (e.g., sedatives and other psychotropic agents), the increase in body fat with aging will result in a larger Vd. Greater storage of drug in fat can lead to drug accumulation over time and a longer serum half-life. Drug accumulation can lead to drug toxicity. A lower initial dose or a dose reduction after a period of time may be required to avoid toxicity. - plasma protein binding
Aging results in a fall in mean serum albumin levels, from about 40 g/L, at age 40, to approximately 36 g/L, in those 80 or older. This is significant for highly protein bound drugs (e.g., phenytoin).With a decrease in plasma protein (albumin), the percentage of drug in serum that is bound to protein is reduced and the percentage of drug that is free (unbound) is increased. It is the free drug that has a pharmacologic action. Reduced plasma albumin levels have been shown to be responsible for greater unbound drug fractions in the elderly. This is most important for drugs that are extensively bound to plasma albumin.The concurrent administration of two highly bound drugs that compete for the same plasma protein binding sites is more likely to result in an increased effect of each in the elderly. This is particularly so if one or more of the drugs has a narrow therapeutic index, such as digoxin or warfarin.
- volume of distribution
-
3) Drug elimination
Drugs are eliminated from the body primarily by renal excretion or liver metabolism. Both of these processes can be affected by aging.
-
-
- renal excretion of drugs
Renal function declines with age due to many changes in renal structure and function. For drugs eliminated by the kidney, reduced renal function is probably the single most important factor responsible for drug accumulation, resulting in elevated serum levels and increased drug action in the elderly.Both the excretory functions of the kidney and its ability to maintain the composition of body fluids are affected by aging. After the fourth decade, there is a progressive decline of about 10 percent per decade in the total renal blood flow and glomerular filtration rate. By age 80, renal function is approximately 50% of that seen in a 40 year old person.Serum creatinine values are often used to reflect the state of renal function. An increase in serum creatinine signifies decreased glomerular filtration rate (GFR). Serum creatinine can be maintained in the normal range until kidney function falls below 50% of normal. In the elderly, however, renal function may fall without producing a corresponding increase in serum creatinine because of a decrease in creatinine production. Therefore, for dosing purposes, the creatinine clearance is adjusted according to age.In young adults, the normal creatinine clearance is 125 mL/min (2 mL/sec). Dose adjustment is usually required for drugs that are renally eliminated when the creatinine clearance falls below the 30-50 mL/min range. The exact information is published by each manufacturer.As a result of a reduced renal function, the dosage of many drugs that are eliminated primarily by the kidney (e.g., digoxin, acyclovir, lithium) must be reduced to prevent accumulation in the elderly patient.
- hepatic metabolism of drugs
Liver size and blood flow decline with age. The decline in the liver’s ability to metabolize drugs depends on the metabolic route. Oxidation and reduction reactions (Phase I metabolism) involving the cytochrome P450 enzyme system decline with age. Conjugation reactions (Phase II metabolism) remain unchanged.The consequences of reduced metabolism will depend on the drug concerned. If the drug is inactivated by metabolism, a reduction in hepatic metabolism should increase the duration of action of the drug. If bioavailability depends on the quantity of the drug able to escape “first-pass” metabolism, a reduction in liver metabolism should be reflected in increased initial serum levels of the drug and possibly also a longer half-life. If, on the other hand, a drug is activated by first-pass metabolism in the liver, it may have a reduced effect in the elderly patient with liver impairment. Examples of prodrugs are enalapril (active metabolite enalaprilat) and codeine (active metabolite morphine).
- renal excretion of drugs
-
Liver Disease
Liver disease tends to be seen more often in the older patient.
The changes that occur in liver disease can affect drug absorption, distribution, metabolism and elimination of a number of drugs. Some liver diseases affect protein concentrations in the blood (albumin is made in the liver), which can alter the extent of protein binding of certain drugs. Other liver diseases (e.g., cirrhosis) may reduce blood flow to the liver, or drug metabolizing capacity.
Doses of drugs that are eliminated primarily by the liver often need to be adjusted in hepatic insufficiency such as that seen in severe alcoholic cirrhosis. Recommendations for dosage adjustment in liver disease can be found in the drug product monograph, and in general take the following factors into consideration:
-
-
- the severity of liver disease
- the portion of total drug clearance performed by the liver (versus that contributed by the kidneys)
- the route of administration
- the duration of therapy
-
Dosage adjustment is usually required if:
-
-
- liver disease is severe
- metabolizing capacity of the liver is decreased
- the drug has a narrow therapeutic range
- the drug is to be administered on a chronic basis
-
Renal Impairment
Kidney disease is not unique to the elderly population, but some degree of renal impairment is often seen in this patient group.
The elimination of drugs that are primarily excreted unchanged by the kidney (i.e., not extensively metabolized by the liver) is greatly reduced in patients with renal insufficiency. As well, it is important to note that the absorption, distribution, and metabolism and elimination of drugs that are eliminated by other routes (i.e., by liver metabolism) may be affected by kidney disease.
Drug absorption in patients with renal failure may be altered due to changes in gastrointestinal emptying time, gastric pH or edema of the gastrointestinal tract.
The volume of distribution of many drugs may be altered in patients with renal failure.
The metabolism of some drugs may also be altered in patients with renal insufficiency. This may occur as a result of decreased metabolism of drugs by the kidney itself or due to a reduction in renal elimination of the metabolic products of liver metabolism. Decreased renal elimination of the products of liver metabolism (i.e., metabolites) can result in drug toxicity (e.g., morphine is metabolized in the liver, but its metabolites are excreted by the renal route).
In order to maintain a serum concentration of a drug in a patient with renal insufficiency that is similar to a patient with normal renal function, the dose must be adjusted. Two methods exist to accomplish this:
-
-
- interval prolongation method – dose is kept the same but the interval between doses is lengthened
- dose reduction method – dose is reduced but the interval between doses is kept the same
-
A combination of these two strategies may also be used.
Medications that are renally eliminated and have a narrow therapeutic index should be used with caution in persons with renal impairment. For example, the aminoglycoside antibiotics may worsen renal impairment or may produce ototoxicity*.
A medication may be selected for use in a person with renal impairment because it is completely eliminated by another route. For example, ceftriaxone is eliminated by the liver and can be given without dosage adjustment to patients with poor renal function. Recommendations for dosage adjustment in renal impairment can be found in the drug monograph.
Pharmacodynamics
End organ responsiveness may be affected by:
-
-
- alteration of receptor site(s) and/or altered responsiveness of receptors with age
- decreased number of neurons and neurotransmitters
- changes in homeostatic responses
- organ pathology
- changes in body composition leading to elevated drug concentration at the receptor site
- acute illness
-
1) Drug sensitivity
The elderly can be inherently more sensitive to drugs as witnessed by:
-
-
- sedation from benzodiazepines is greater in the elderly
- the hypotensive effects of vasodilators are enhanced in some older patients
- the analgesic and sedative properties of opiates are greater in the elderly
- the anticoagulant effects of warfarin are increased
- anticholinergic drugs can cause cognitive impairment
-
Sedatives, antipsychotics, antidepressants, anticholinergic agents, antihypertensives, and digoxin should all be started at reduced dosages and slowly titrated upwards if needed. Anticholinergic drugs should be used cautiously in the elderly.
2) Adverse drug reactions
Some common adverse drug reactions seen in the elderly patient include:
-
-
- oversedation from sedatives
- gastrointestinal irritation, ulceration, hemorrhage
- constipation
- delirium
- voiding problems (either incontinence or urinary retention)
-
Patients at highest risk of experiencing adverse drug reactions include individuals:
-
-
- on multiple medications
- on medications with a narrow therapeutic index
- over 70 years of age
- with significant cardiovascular problems (present or previous congestive heart failure)
- with reduced hepatic function
- with renal insufficiency
- with malnutrition
-
Polypharmacy
Although seniors represent approximately 13% of Canada’s population, they account for approximately 30 to 40% of all prescriptions. Approximately 80% of all seniors living at home use some form of prescription or over-the-counter medication. Over 50% of these use two or more medications.
Unnecessary prescribing, misuse of medication and inappropriate prescriptions increase the risk of drug-related illness. An estimated 6% to 28% of hospital admissions among the elderly are due to drug-related illness.
Polypharmacy may be a result of inappropriate prescribing. Some of the drugs may have been prescribed by different physicians who are unaware of all the medications being taken by an individual. Elderly patients may present frequently to their doctors with a variety of ailments for which they are seeking treatment with medications. Seniors may also be taking herbal remedies or other non-prescription drugs that interact in unpredictable ways.
Another reason for increased drug use is that the use of preventive approaches to disease management have increased in the last decade. Examples include:
-
-
- ASA and other agents for stroke prevention
- bisphosphonate and other agents for prevention of osteoporosis
- antihypertensives and cholesterol-lowering agents for prevention of cardiovascular events
- ACE inhibitors for patients with diabetes mellitus for prevention of kidney damage
-
Regular medication review may reduce the number of drugs required and may reduce the risk of adverse effects due to simultaneous use of several drugs. Clinicians use explicit criteria (e.g., Beers criteria-list of medications to avoid in the elderly generally) and implicit criteria (consideration of all factors affecting drug action in an individual such as the pharmacokinetic and pharmacodynamic changes that occur in the elderly and drug interactions).
Most pharmacists keep computerized records of the prescriptions a person is taking and can help to monitor drug duplication or potential for drug interactions.
Compliance
The elderly may have difficulty adhering to a treatment regimen due to a number of factors, such as:
-
-
- increased prevalence of memory disorders
- visual impairment
- complex drug regimens
- inadequate knowledge about the drug, its purpose and the duration of therapy
-
Health care workers can help improve compliance in the elderly by providing:
-
-
- a review of medications to ensure that all are essential
- clear verbal instructions
- clearly written supplemental information
- non-childproof, easily opened containers when dispensing (for patients with arthritis of the hands)
- medication reminder systems (e.g., pill organizer boxes)
-
Practices such as hoarding medications for later use and using medications prescribed for other individuals are dangerous and should be discouraged.
Summary — Section 2: Drug Dosing in the Elderly
Effective drug use in the elderly can greatly enhance the quality of life of the patient. However, the elderly patient is often taking multiple medications for concomitant disorders, and the risks of adverse reactions associated with medications are greater in an older population.
The following effects of aging on the absorption, distribution, and metabolism and excretion of medications must be recognized, and dosages must be adjusted accordingly to avoid adverse effects:
-
-
- absorption – decreased acid secretion, gastric motility and first-pass metabolism
- distribution – altered volume of distribution and decreased plasma protein binding
- renal elimination – declining renal function will impair the elimination of drugs that are eliminated by the kidney and the elimination of liver metabolites that are eliminated through the kidney
- liver metabolism – oxidative metabolism (P450 enzyme system) may be reduced. Metabolism by glucuronidation may be maintained.
-
Because the elderly generally have more chronic disorders and also may present to their doctors with a variety of ailments from time to time, concomitant drug use is more common than in other age groups. The advent of new preventive approaches to diseases also increases the likelihood of the elderly taking multiple medications. These situations could lead to increased adverse reactions, polypharmacy, and/or noncompliance. Clinicians use explicit and implicit criteria to assess the appropriateness of drug therapy in the elderly.
Compliance may be improved by:
-
-
- minimizing the number of medications
- simplifying the regimen
- educating the patient
- using compliance aids
- improving the physician-patient relationship
-
Appropriate prescribing takes all of these factors into consideration.
Progress Check — Section 2: Drug Dosing in the Elderly
1.
Achlorhydria may reduce the amount of weakly acidic drug absorbed from the stomach.
a) true
b) false
2.
In elderly patients:
a) total body water increases
b) the volume of distribution for most water soluble drugs is decreased
c) serum albumin levels increase
d) the unbound fraction of drug decreases
3.
Indicate whether each of the following is true or false.

4.
Dosage adjustment is usually required in liver disease if:
a) the disease is severe
b) the drug metabolism is not changed
c) the drug has a wide therapeutic range
d) the frug is to be administered on an acute basis only
5.
What methods of dosage adjustment are used in patients with renal insufficiency?
_______________________________
_______________________________
_______________________________
_______________________________
6.
What criteria do clinicians use to assess the appropriateness of drug therapy in the elderly?
_______________________________
_______________________________
_______________________________
_______________________________
7.
What are some methods that are available to improve drug compliance with seniors?
_______________________________
_______________________________
_______________________________
_______________________________
Progress Check Answers — Section 2: Drug Dosing in the Elderly
1.
a) true
2.
b) the volume of distribution for most water soluble drugs is decreased
3.
1) False
In the elderly, renal function may fall without producing a corresponding increase in serum creatinine.
2) True
3) True
4) True
5) False
The consequences of reduced metabolism will depend on the drug concerned and the existence of alternate elimination pathways.
6) False
The absorption, distribution and metabolism and elimination of drugs that are eliminated by other routes (i.e., by liver metabolism) may be affected by kidney disease.
4.
a) the disease is severe
5.
Interval prolongation method
Dose reduction method
6.
explicit criteria – e.g., Beers list of medications to avoid
implicit criteria – pharmacokinetic and pharmacodynamic factors affecting the individual
7.
Compliance may be improved by:
-
-
- minimizing the number of medications
- simplifying the regimen
- educating the patient
- using compliance aids
- improving the physician-patient relationship
-
References
Beers MH. Explicit criteria for determining potentially inappropriate medication use by the elderly: an update. Arch Intern Med 1997;157:153-6.
Fick DM. Cooper JW. Wade WE. Waller JL. Maclean JR. Beers MH. Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts. Archives of Internal Medicine. 2003;163(22):2716-24
Shelton PS, Fritsch MA, Scott MA. Assessing medication appropriateness in the elderly, a review of available measures. Drugs Aging 2000;16(6):437-450.
Section 3: Demographics
Learning Objectives
After reading this section you should be able to:
- State the percentage of Canada’s population that is elderly.
- Explain the reasons for the increasing senior population in Canada.
- Identify the life expectancy of Canadian seniors.
- Identify the leading chronic health conditions and the leading causes of death of Canadian seniors.
- Identify the percentage of Canadian seniors that require use of medications.
Canada’s Seniors
Seniors are one of the fastest growing population groups in Canada. Of the 30 million Canadians in 2001, 3.9 million were 65 and older. This represents about 13% of our population. This number will continue to increase in the coming years to 14.6% in 2010 and 22% by 2031. (Source: Division of Aging and Seniors, Health Canada)
Factors Contributing to an Increased Number of Elderly
Several factors are responsible for the increase in Canada’s aging population.
1) Baby Boomers
The baby boomers born from 1946 to 1966 start turning 65 beginning in 2011. A dramatic increase in the number of seniors will occur over a short 20 year span from that point in time.
2) Decreased fertility rate
Because families are having fewer children, seniors represent a larger percentage of the population.
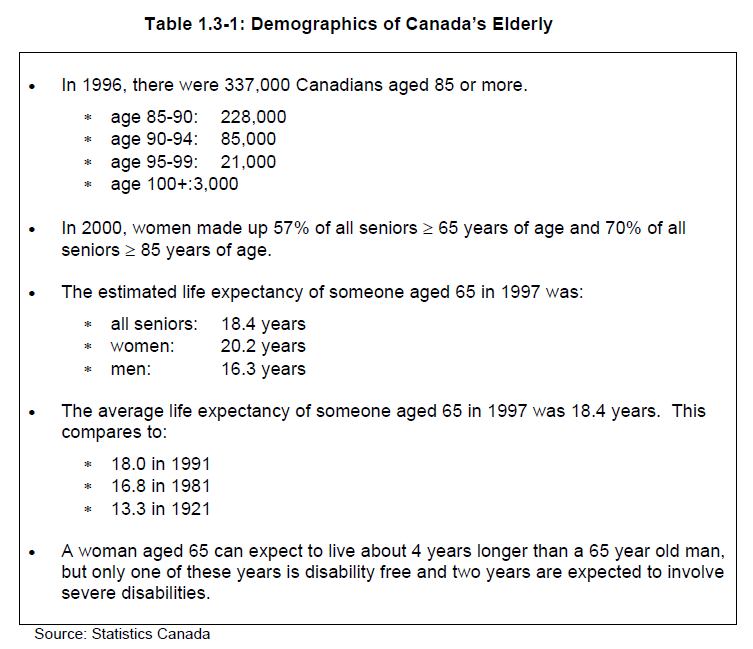
3) Increased life expectancy
People are living longer. The average life expectancy of a Canadian aged 65 has been gradually increasing (see Table 1.3-1). Life expectancy is now 5 years more than it was in 1921. Women live longer than men.
Seniors aged 85 and over represent the fastest growing segment of the senior population.
4) Reduced mortality rate
At the same time as life expectancy has been increasing, the age-related mortality rates have been decreasing due to improved living conditions, health care, and lifestyles. The major cause of mortality is now chronic disease rather than infectious disease.

Morbidity and Mortality of Seniors
A high percentage of seniors living at home have a chronic health condition and approximately one-quarter have long-term disabilities (see Table 1.3-2). Women live longer than men but women spend more of their later years disabled.
The leading chronic health conditions are:
-
-
- arthritis or rheumatism
- high blood pressure
- food/other allergies
- heart disease
- back problems
- diabetes
- cataracts
- incontinence
- glaucoma
-
A substantial number of seniors suffer from chronic pain or discomfort.
The presence of concurrent multiple chronic diseases is more prevalent with advancing age. Disability and disease affect the ability of seniors to carry out daily living activities, and impede on their independence plus impact on the need for long-term care.
Depression is a significant problem in the elderly and is under-diagnosed. Other neurologic diseases affecting the elderly include Parkinson’s disease and dementia*.
Seniors are generally far more likely than individuals aged 45-64 to be hospitalised. Hospitalization rates rise substantially for older seniors. Seniors also tend to stay in the hospital for considerably longer periods than younger people.
The four leading causes of death of seniors are:
-
-
- coronary heart disease
- lung cancer
- stroke
- respiratory diseases
-
Although the death rate from heart disease among seniors has been decreasing (34% lower in 1996 than in 1980), the cancer death rate rose 9% over the same period of time.
Summary — Section 3: Demographics
Approximately 13% of Canada’s population is age 65 or older. Canada’s population is aging due to decreased fertility rates, aging baby boomers, increased life expectancy, and decreased mortality rates.
The average life expectancy of someone aged 65 in 1996 was 18.4 years. Women live longer than men, but are not necessarily healthier than men in their senior years.
Over 80% of all seniors living at home have a chronic health condition and many seniors use two or more medications. The nine leading chronic health conditions are:
-
-
- arthritis or rheumatism
- high blood pressure
- food/other allergies
- heart disease
- back problems
- diabetes
- cataracts
- incontinence
- glaucoma
-
Important neurologic diseases affecting the health of Canada’s elderly include depression, Parkinson’s disease and dementia.
The four leading causes of death of seniors are:
-
-
- coronary heart disease
- lung cancer
- stroke
- respiratory diseases
-
Progress Check — Section 3: Demographics
1.
Indicate whether each of the following statements is True or False.

2.
List 5 leading chronic health conditions of seniors.
1 _________________________________
2 _________________________________
3 _________________________________
4 _________________________________
5 _________________________________
3.
What are the 4 leading causes of death of seniors?
__________________________________
__________________________________
__________________________________
__________________________________
Progress Check Answers — Section 3: Demographics
1.
1) True
2) True
3) True
4) False
Over 60% of seniors use two or more medications.
2.
Any 5 of the following:
-
-
- arthritis or rheumatism
- high blood pressure
- food/other allergies
- heart disease
- back problems
- diabetes
- cataracts
- incontinence
- glaucoma
-
3.
coronary heart disease
lung cancer
stroke
respiratory diseases
Module 1 Test
1.
With normal aging, which of the following occur? Select all that apply.
_____ a) thickening of left ventricular wall of the heart
_____ b) increased heart rate
_____ c) decline in number of neurotransmitters
_____ d) decreased glucose tolerance
_____ e) decreased bone density
_____ f) decreased cellular immunity
_____ g) increased renal blood flow
_____ h) increased acidity of urine
2.
The elderly patient usually has:
a) a decrease in acid secretion in the stomach
b) an increase in gastric motility
c) an increase in total body water
d) an increase in serum albumin levels
3.
The most important factor responsible for altered drug levels and increased drug action in the elderly is:
a) delayed gastric emptying
b) decreased plasma protein binding
c) reduced renal function
d) reduced hepatic metabolism
4.
Patients at highest risk of experiencing adverse drug reactions include individuals:
a) on multiple medications
b) over 70 years of age
c) with significant cardiovascular problems
d) all of the above
5.
Seniors represent approximately 20% of the Canadian population.
a) true
b) false
6.
Which of the following statements is true?
a) Seniors represent a larger percentage of the population than they did 10 years ago.
b) Seniors aged 85 and over represent the fastest growing segment of the senior population.
c) Approximately 75% of all seniors living at home use some form of prescription or over-the-counter medication.
d) all of the above
7.
Which of the following are leading chronic health conditions of seniors?
_____ a) liver disease
_____ b) arthritis
_____ c) cataracts
_____ d) high blood pressure
_____ e) heart disease
_____ f) incontinence
_____ g) gout
_____ h) diabetes
_____ i) back problems
_____ j) psoriasis
_____ k) glaucoma
_____ l) food/other allergies
8.
What are the four main causes of death of seniors?
_____ a) lung cancer
_____ b) heart disease
_____ c) stroke
_____ d) accident
_____ e) respiratory disease
_____ f) infectious disease
_____ g) diabetes
Module 1 Test Answers
1.
a) thickening of left ventricular wall of heart
c) decline in number of neurotransmitters
d) decreased glucose tolerance
e) decreased bone density
f) decreased cellular immunity
2.
a) a decrease in acid secretion in the stomach
3.
c) reduced renal function
4.
d) all of the above
5.
b) false
6.
d) all of the above
7.
b) arthritis
c) cataracts
d) high blood pressure
e) heart disease
f) incontinence
h) diabetes
i) back problems
k) glaucoma
l) food/other allergies
8.
a) lung cancer
b) heart disease
c) stroke
d) respiratory disease
